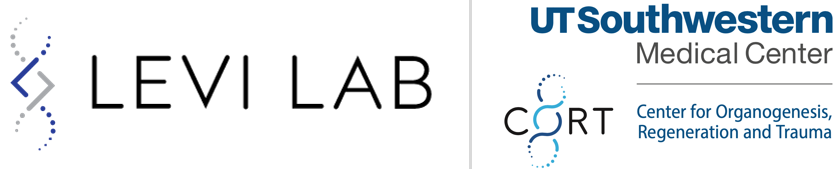The Levi laboratory is proud to present a publication in Nature Communications entitled “Regulation of heterotopic ossification by monocytes in a mouse model of aberrant wound healing.”
While experts suspected that heterotopic ossification was somehow linked to inflammation, new research from the Levi Laboratory explains how this happens on a cellular scale—and suggests a way it can be stopped. To help explain how the healing process goes awry in heterotopic ossification, the research team, led by Levi, Michael Sorkin, M.D. and Amanda Huber, Ph.D., of the Department of Surgery’s section of plastic surgery, took a closer look at the inflammation process in mice. Using tissue from injury sites in mouse models of heterotopic ossification, they used single cell RNA sequencing to characterize the types of cells present. They confirmed that macrophages were among the first responders and might be behind aberrant healing. Upon closer examination, the Michigan team found that macrophages are more complex than previously thought—and don’t always do what they are supposed to do. Specifically, during heterotopic ossification formation, the increased presence of macrophages that express TGF-beta leads to an errant signal being sent to bone forming stem cells. Working with the lab led by Stephen Kunkel, Ph.D. of the Department of Pathology, the team demonstrated that an activating peptide to CD47, p7N3 could alter TGF-beta expressing macrophages, reducing their ability to send signals to bone-forming stem cells that lead to heterotopic ossification. The team hopes to eventually develop translational therapies that target this pathway and further characterize not just the inflammatory cells but the stem cells responsible for the abnormal bone formation. Special thank yous to the University of Michigan Department of Surgery and Section of Plastic Surgery, Center for Molecular Imaging, and the rest of the Levi laboratory team.
PMID: 32024825. (Read here!)
Abstract
Heterotopic ossification (HO) is an aberrant regenerative process with ectopic bone induction in response to musculoskeletal trauma, in which mesenchymal stem cells (MSC) differentiate into osteochondrogenic cells instead of myocytes or tenocytes. Despite frequent cases of hospitalized musculoskeletal trauma, the inflammatory responses and cell population dynamics that regulate subsequent wound healing and tissue regeneration are still unclear. Here we examine, using a mouse model of trauma-induced HO, the local microenvironment of the initial post-injury inflammatory response. Single cell transcriptome analyses identify distinct monocyte/macrophage populations at the injury site, with their dynamic changes over time elucidated using trajectory analyses. Mechanistically, transforming growth factor beta-1 (TGFβ1)-producing monocytes/macrophages are associated with HO and aberrant chondrogenic progenitor cell differentiation, while CD47-activating peptides that reduce systemic macrophage TGFβ levels and help ameliorate HO. Our data thus implicate CD47 activation as a therapeutic approach for modulating monocyte/macrophage phenotypes, MSC differentiation and HO formation during wound healing.